Chapter 1: The science and the scan
"Boring, But Necessary"
- Hybrid Imaging System
- Anatomic & Functional Exam
- The Machine
- “Whole Body” vs. “Skull Base to Mid-Thigh”
- Three Sets of Images
Produced
- Glucose Analog
- Malignancy & Glucose Metabolism
- Mechanisms for Increased Intracellular Glucose
- Why 18F-FDG Works
- Whole Body Assessment
- The “You’re Kidding Me!” Effect
- Post-Therapeutic Scar vs. Active Malignancy
- Detecting Malignancy
- Staging Malignancy
- Assess Response to Therapy
- Detecting Recurrence
- Not All Cancer is FDG-Avid
- Normal FDG-Uptake vs. Pathologic Uptake
- Technical Limitations
- Poor Patient Preparation
- Misregistration
- Brown Fat Activation
- SUV Problems
- Fields of View Discrepancy
- PET/CT Artifacts
- Timing of Exam After Therapy
- CT Images
- Non-Attenuation Corrected Images
- Attenuation Corrected Images
- Maximum Intensity Projection (MIP)
- Fusion of Images
- All Images Viewed in 3 Planes
7. Contrast Media: Oral & I.V.
- Who Gets Oral Contrast?
- Who Gets IV Contrast?
- Oral Contrast “Cocktail” Recipe
8. What the Patient Should Expect
- Documenting Height & Weight
- Private Resting Room
- Drinking PO Contrast
- FDG Injection
- Delay Between Injection & Scan
9. Safety Concerns with PET/CT Imaging
- Radiation Exposure to Patient
- Radiation Exposure to Patient’s Contacts
- Patient Contact with Pregnant Women
- Breastfeeding
Chapter 2: PET/CT Problems Which Limit Interpretation
"Something just doesn't seem right here"
- Optimizing Glucose & Insulin Levels
- Fasting Prior to Exam
- Diabetic Patients
- Low Carbohydrate Diet
- Hydration
- Strenuous Exercise
- Voiding Prior to Exam
- Patient Instruction Sheet
- Definition
- Distribution / Appearance
- Don’t Miss the Hidden Nod
- Reporting Language
- Prevention
3. Timing of PET/CT Exam After Therapy
- “Rule of 3”
- Chemotherapy: 1 month
- Surgery: 2 months
- Radiation: 3 months
- Etiology: Hybrid Imaging
- Patient Movement
- Respiratory Motion
- Breathing Techniques
- Bowel Peristalsis
- False Positives
- False Negatives
- Reporting Language
- Beam Hardening
- Diaphragmatic Mismatch
- Linear Hand Motion
- Attenuation Correction
- Differing Fields of View
- Poor Patient Preparation
- FDG Extravasation
- Extensive Brown Fat
- Metformin-Induced Bowel Uptake
- Marked Reactive Marrow Uptake
- Extensive Tumor Uptake in
- Different Types of SUV Measurements
- Factors that Influence SUV Measurements
- What SUV Number Indicates Malignancy?
- What Percent Change in SUV on a Follow Up Exam is Significant?
- How to Compare Exams With Very Different Background Metabolic Activities?
Chapter 3: The Standardized Uptake Value (SUV)
"The good, the bad & the ugly"
1. What is the SUV & Why Used?
- Quantitative vs. Qualitative Assessment
- Unitless Measurement
- Formula
- SUV = ?
- Patient Preparation
- Time Between FDG Injection & Scan
- Partial Volume Effects
- Extravasation
- Patient Weight
- Size & Position of ROI
- Attenuation Correction Artifacts
- Consensus?
- Body Weight
- Lean Body Mass
- Ideal Body Weight
- Body Surface Area
- Maximum vs. Mean
- Average SUV’s by Organ
4. Interpreting the SUV: Threshold Values, “Oncologic Plausibility” & Relative Uptake
- Precise Threshold Values?
- “Oncologic Plausibility”
- Relative Uptake
- Assessing Nodes in Lymphoma Cases
- Assessing Nodes in Non-Lymphoma Cases
- Potential Lesions in Solid Organs
- Pulmonary Nodules
5. What % Change in SUV on a Follow Up Exam is Clinically Significant?
- The Problem
- Current Recommendations
6. How to Compare Sequential Exams With Very Different Background Activities?
- Differing Background Metabolic Activities
- When Qualitative Assessment is Required
- Reporting Language
7. Should We Just Abandon the SUV?
- Pros & Cons
- “Qualitative” Definitions
- Mild
- Moderate
- Intense
- Final Recommendations
Chapter 4: Our Systematic Approach to Reading a PET/CT
"Eat your vegetables"
1. Reading Station & Reading Software
- Reading Station
- Monitor Set-Up
- PET/CT Reading Software
- Hanging Protocol
- Reading in Context (“Oncologic Plausibility”)
- Measure Size on CT, Not on PET Images
- Abnormality Seen Only on First PET Image
- Assess the Patient’s Main Pathology Last
- Beware the Ureter
3. Excellent Views: The MIP, Coronal & Sagittal Images
- 3-D Rotating MIP & Coronal “Quick MIP”
- Coronal PET
- Sagittal PET
4. Written Annotations While Reading
- Numbers, Numbers & More Numbers
- Size & SUV Annotation System
- Sample Annotation Sheet
- Goals of Reporting
- Lawyers, Lawyers & Lawyers
- Sample PET/CT Report
- Negative Exam
- Positive Exam
- Patient Questionnaire
- Technologist’s Data Sheet
- Huge Exam: Requires Systematic Approach
- Our “12-Step Reading System”
- “The Read” in Action: Sample Case (Video)
- Annotations for Sample Case
- Final Report for Sample Case
Chapter 5: Normal Physiologic Distribution of FDG
"The essentials"
- To Locate Cancer, First Eliminate:
- Normal FDG-Avid “Structures”
- Benign FDG-Avid “Findings”
Chapter 6: Benign FDG-Avid "Findings" & Common Diagnostic Challenges
"Separating the Expert from the Not-So-Expert"
3. Chest
- Inflammatory Lymph Nodes
- Thymic Rebound
- Pleura: Talc Pleurodesis vs. Malignancy vs. Inflammation
-
Radiation-Induced Lung Disease
- Radiation Pneumonitis
- Radiation Fibrosis
- "Post-Therapeutic Inflammatory Changes" / Scarring of the Lung
- Atelectasis / Infiltrate
- Lipomatous Hypertrophy of the Inter-Atrial Septum
- Elastofibroma Dorsi
- Site of Prior Chest Port
- Esophagitis vs. Neoplasm
- Subcutaneous & Intramuscular Medical Injections
- Injected FDG-Blood Clot
4. Abdomen & Pelvis
- The Heterogeneous Liver
- Liver Ablation
- Hypermetabolic Geographic Fatty Infiltration
- Hypermetabolic Hepatic Adenoma
- FDG-Avid Adrenal Gland Algorithm
- Therapy-Induced Splenic Activation
- Peritoneal Carcinomatosis
- Pre-Sacral Soft Tissue After Rectal Surgery
- Gallbladder: Cholecystitis vs. Malignancy
- Inguinal Herniorraphy
- Bladder in Inguinal Canal
- Uterine Fibroid
- Tampon
5. Miscellaneous (continued)
-
Vascular Uptake
- Atherosclerosis
- Vasculitis
- Vascular Grafts
-
Value of NAC PET Images
- Resolving AC Artifacts
- Lung Nodule Identification
-
Non-Malignant, Yet Clinically Significant, FDG-Avid CT Abnormalies
- Acute Diverticulitis
- Colitis
- Cholecystitis
- Pneumonia
- Abscess
- Pancreatitis
- Skeletal Abnormalities [See Chapter 7]
Chapter 7: The Bones
"...is connected to the..."
Chapter 8: The Cancers
"Putting it all together"
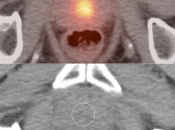
Prostate Cancer
Fast Facts:
- Most common cancer of US men (1:7)
- 2nd leading cause of cancer death for US men
- Stage I & 2: 5-yr survival > 95%
Normal Prostatic Uptake:
- The normal prostate typically demonstrates little or no FDG uptake.
- Mild diffuse prostate uptake is considered normal.
- Moderate or intense diffuse uptake typically reflects prostatitis.
- Although even focal FDG uptake in the prostate is often normal, correlation with PSA levels is advised, especially if the uptake is located in the peripheral zone (location of 70% of prostate cancers).
- Uptake centrally in the gland typically represents normal hypermetabolic urine in the prostatic urethra.
Increased Incidence of Malignancy:
- Uptake associated with a visible lesion or area of focal calcification the CT exam.
- Focal uptake located in the peripheral zone.
- The presence of associated hypermetabolic nodes or bone lesions.
Distant Disease: Most commonly to the bones, lymph nodes, lung, liver and brain.
Indications for PET/CT Imaging:
Screening, Diagnosis & Initial Staging:
- Due to the poor FDG avidity of many prostate cancers, the overlap of increased uptake often associated with prostatitis, the marginal sensitivity of detecting pelvic nodal disease and the limitations created by superimposition of intense bladder activity, PET/CT currently has no role in the screening or diagnosis of prostate cancer. For similar reasons, it is generally of limited utility for initial staging of the disease.
Utility of PET/CT:
- Detection of local recurrence and/or metastatic disease in patients with “PSA Relapse” or “Biochemical Failure”.
- Monitoring response to androgen deprivation therapy.
- Assessing extent of metabolically active castrate-resistant disease.
- Assessing quiescent versus metabolically active osseous metastatic disease.
- Prognosis assessment.
- Directing re-biopsy (if initial results are negative in the setting of a high clinical suspicion of malignancy).
- MRI is considered a better modality for both initial assessment of extracapsular and seminal vesicle involvement, as well as for evaluation of recurrence in the prostatic bed.
What We Report:
Size, metabolic activity & location for the primary lesion (if visualized) and representative metastatic lesions.
- Primary Lesion: Often not identified. When present, usually appears as a focus of intense uptake in the peripheral zone (MRI is superior in the evaluation of the primary lesion).
- Regional Disease: Usually hypermetabolic pelvic lymph nodes.
- Distant Disease: Most commonly to the bones, lymph nodes, lung, liver and brain.
Bone Scan versus PET/CT for Osseous Metastases:
PET/CT imaging has traditionally been considered less sensitive than a conventional bone scan for blastic metastases (e.g. prostate & breast cancers).
Recent literature, however, suggests that while a bone scan may be more sensitive than a PET scan alone for blastic lesions, it may be actually less sensitive when compared to a PET scan plus a CT scan (e.g. a PET/CT scan).
False Positives:
- Benign prostatic hyperplasia
- Prostatitis
- Prostatic urethra (if urine present)
False Negatives:
- Primary and metastatic lesions < 8.0 mm (“beneath the resolution of PET”)
Additional Radiotracers:
Pending further investigation, C-11 Acetate, C-11 Choline, F-18 Choline, C-11 Methionine, F-18 Fluorocholine and F-18 Sodium Fluoride may prove useful in PET/CT prostate imaging.