Chapter 1: The science and the scan
"Boring, But Necessary"
- Hybrid Imaging System
- Anatomic & Functional Exam
- The Machine
- “Whole Body” vs. “Skull Base to Mid-Thigh”
- Three Sets of Images
Produced
- Glucose Analog
- Malignancy & Glucose Metabolism
- Mechanisms for Increased Intracellular Glucose
- Why 18F-FDG Works
- Whole Body Assessment
- The “You’re Kidding Me!” Effect
- Post-Therapeutic Scar vs. Active Malignancy
- Detecting Malignancy
- Staging Malignancy
- Assess Response to Therapy
- Detecting Recurrence
- Not All Cancer is FDG-Avid
- Normal FDG-Uptake vs. Pathologic Uptake
- Technical Limitations
- Poor Patient Preparation
- Misregistration
- Brown Fat Activation
- SUV Problems
- Fields of View Discrepancy
- PET/CT Artifacts
- Timing of Exam After Therapy
- CT Images
- Non-Attenuation Corrected Images
- Attenuation Corrected Images
- Maximum Intensity Projection (MIP)
- Fusion of Images
- All Images Viewed in 3 Planes
7. Contrast Media: Oral & I.V.
- Who Gets Oral Contrast?
- Who Gets IV Contrast?
- Oral Contrast “Cocktail” Recipe
8. What the Patient Should Expect
- Documenting Height & Weight
- Private Resting Room
- Drinking PO Contrast
- FDG Injection
- Delay Between Injection & Scan
9. Safety Concerns with PET/CT Imaging
- Radiation Exposure to Patient
- Radiation Exposure to Patient’s Contacts
- Patient Contact with Pregnant Women
- Breastfeeding
Chapter 2: PET/CT Problems Which Limit Interpretation
"Something just doesn't seem right here"
- Optimizing Glucose & Insulin Levels
- Fasting Prior to Exam
- Diabetic Patients
- Low Carbohydrate Diet
- Hydration
- Strenuous Exercise
- Voiding Prior to Exam
- Patient Instruction Sheet
- Definition
- Distribution / Appearance
- Don’t Miss the Hidden Nod
- Reporting Language
- Prevention
3. Timing of PET/CT Exam After Therapy
- “Rule of 3”
- Chemotherapy: 1 month
- Surgery: 2 months
- Radiation: 3 months
- Etiology: Hybrid Imaging
- Patient Movement
- Respiratory Motion
- Breathing Techniques
- Bowel Peristalsis
- False Positives
- False Negatives
- Reporting Language
- Beam Hardening
- Diaphragmatic Mismatch
- Linear Hand Motion
- Attenuation Correction
- Differing Fields of View
- Poor Patient Preparation
- FDG Extravasation
- Extensive Brown Fat
- Metformin-Induced Bowel Uptake
- Marked Reactive Marrow Uptake
- Extensive Tumor Uptake in
- Different Types of SUV Measurements
- Factors that Influence SUV Measurements
- What SUV Number Indicates Malignancy?
- What Percent Change in SUV on a Follow Up Exam is Significant?
- How to Compare Exams With Very Different Background Metabolic Activities?
Chapter 3: The Standardized Uptake Value (SUV)
"The good, the bad & the ugly"
1. What is the SUV & Why Used?
- Quantitative vs. Qualitative Assessment
- Unitless Measurement
- Formula
- SUV = ?
- Patient Preparation
- Time Between FDG Injection & Scan
- Partial Volume Effects
- Extravasation
- Patient Weight
- Size & Position of ROI
- Attenuation Correction Artifacts
- Consensus?
- Body Weight
- Lean Body Mass
- Ideal Body Weight
- Body Surface Area
- Maximum vs. Mean
- Average SUV’s by Organ
4. Interpreting the SUV: Threshold Values, “Oncologic Plausibility” & Relative Uptake
- Precise Threshold Values?
- “Oncologic Plausibility”
- Relative Uptake
- Assessing Nodes in Lymphoma Cases
- Assessing Nodes in Non-Lymphoma Cases
- Potential Lesions in Solid Organs
- Pulmonary Nodules
5. What % Change in SUV on a Follow Up Exam is Clinically Significant?
- The Problem
- Current Recommendations
6. How to Compare Sequential Exams With Very Different Background Activities?
- Differing Background Metabolic Activities
- When Qualitative Assessment is Required
- Reporting Language
7. Should We Just Abandon the SUV?
- Pros & Cons
- “Qualitative” Definitions
- Mild
- Moderate
- Intense
- Final Recommendations
Chapter 4: Our Systematic Approach to Reading a PET/CT
"Eat your vegetables"
1. Reading Station & Reading Software
- Reading Station
- Monitor Set-Up
- PET/CT Reading Software
- Hanging Protocol
- Reading in Context (“Oncologic Plausibility”)
- Measure Size on CT, Not on PET Images
- Abnormality Seen Only on First PET Image
- Assess the Patient’s Main Pathology Last
- Beware the Ureter
3. Excellent Views: The MIP, Coronal & Sagittal Images
- 3-D Rotating MIP & Coronal “Quick MIP”
- Coronal PET
- Sagittal PET
4. Written Annotations While Reading
- Numbers, Numbers & More Numbers
- Size & SUV Annotation System
- Sample Annotation Sheet
- Goals of Reporting
- Lawyers, Lawyers & Lawyers
- Sample PET/CT Report
- Negative Exam
- Positive Exam
- Patient Questionnaire
- Technologist’s Data Sheet
- Huge Exam: Requires Systematic Approach
- Our “12-Step Reading System”
- “The Read” in Action: Sample Case (Video)
- Annotations for Sample Case
- Final Report for Sample Case
Chapter 5: Normal Physiologic Distribution of FDG
"The essentials"
- To Locate Cancer, First Eliminate:
- Normal FDG-Avid “Structures”
- Benign FDG-Avid “Findings”
Chapter 6: Benign FDG-Avid "Findings" & Common Diagnostic Challenges
"Separating the Expert from the Not-So-Expert"
3. Chest
- Inflammatory Lymph Nodes
- Thymic Rebound
- Pleura: Talc Pleurodesis vs. Malignancy vs. Inflammation
-
Radiation-Induced Lung Disease
- Radiation Pneumonitis
- Radiation Fibrosis
- "Post-Therapeutic Inflammatory Changes" / Scarring of the Lung
- Atelectasis / Infiltrate
- Lipomatous Hypertrophy of the Inter-Atrial Septum
- Elastofibroma Dorsi
- Site of Prior Chest Port
- Esophagitis vs. Neoplasm
- Subcutaneous & Intramuscular Medical Injections
- Injected FDG-Blood Clot
4. Abdomen & Pelvis
- The Heterogeneous Liver
- Liver Ablation
- Hypermetabolic Geographic Fatty Infiltration
- Hypermetabolic Hepatic Adenoma
- FDG-Avid Adrenal Gland Algorithm
- Therapy-Induced Splenic Activation
- Peritoneal Carcinomatosis
- Pre-Sacral Soft Tissue After Rectal Surgery
- Gallbladder: Cholecystitis vs. Malignancy
- Inguinal Herniorraphy
- Bladder in Inguinal Canal
- Uterine Fibroid
- Tampon
5. Miscellaneous (continued)
-
Vascular Uptake
- Atherosclerosis
- Vasculitis
- Vascular Grafts
-
Value of NAC PET Images
- Resolving AC Artifacts
- Lung Nodule Identification
-
Non-Malignant, Yet Clinically Significant, FDG-Avid CT Abnormalies
- Acute Diverticulitis
- Colitis
- Cholecystitis
- Pneumonia
- Abscess
- Pancreatitis
- Skeletal Abnormalities [See Chapter 7]
Chapter 7: The Bones
"...is connected to the..."
Chapter 8: The Cancers
"Putting it all together"
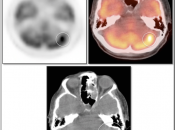
CNS Malignancy (Brain & Spinal Cord)
BRAIN:
- [Imaging of the Sella is covered separately, here]
Fast Facts:
- 2nd leading cause of death for men, ages 20-39
- 5th leading cause of death for women, ages 20-39
- Metastatic lesions are >10 times more common than primary lesions.
Tumor Grade:
While there are many types and subtypes of primary CNS malignant lesions, the PET/CT radiologist can address them as 2 groups:
- “Low-Grade”: Grades I & II (20-80% 5-year survival rate)
- “High-Grade”: Grades III & IV (4-17% 5-year survival rate)
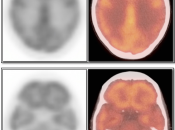
Utility of PET/CT Scan for Primary Brain Tumors:
PET/CT is generally not used to decide whether or not a patient has a primary brain tumor (a diagnosis of brain tumor has nearly always already been made by CT or MRI prior to PET/CT scanning). The true value of PET/CT is determining whether or not a known tumor is “high-grade” or not.
- Characterizing lesions as “low-grade” or “high-grade” (with dramatic implications on management & prognosis):
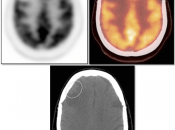
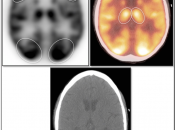
- Low-Grade: Uptake ≈ white matter (may use contralateral centrum semiovale for comparison)
- High-Grade: Uptake > white matter (≈ grey matter)
- As the brain lesion may not clearly identifiable on the non-contrast CT images, it is essential to view the prior MRI (or CT) that lead to the initial diagnosis of “brain tumor”.
- Diagnosis of residual or recurrent tumor.
- Assess potential malignant degeneration of a low-grade lesion to a high-grade lesion.
- Assess response to therapy.
- Direct targeted biopsy of lesion (to its most hypermetabolic area).
- Defining target volumes for radiotherapy.
- Differentiate radiation necrosis (or chemonecrosis) from active malignancy.
Radiation Necrosis (or Chemonecrosis):
- Necrosis presents months to years after radiation therapy (rarely < 3 months post radiation).
- Difficult to differentiate necrosis from malignancy on MRI, as both demonstrate enhancement.
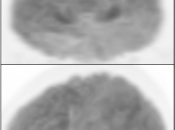
- Necrosis is typically non-avid on PET images.
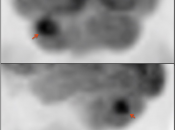
- Recurrent malignancy will demonstrate FDG uptake, often focal and involving only a small portion of a surgical cavity. The uptake may be intense (an easy diagnosis) or may be minimally above adjacent background uptake (a more difficult diagnosis, which may require follow-up).
- FDG-avid recurrence should correspond to the area of enhancement noted on MRI (MRI should be done first, with images available at time of PET/CT interpretation).
- If no evidence of pathologic uptake, we report, “There is no evidence of high-grade tumor recurrence.”
Dual Time Point Imaging:
- Some advocate an additional delayed set of images at 2 hours, as tumor should continue to increase FDG uptake, while normal tissue should plateau.
- The additional time, money, effort, radiation (and questionable utility) dissuade most from employing this technique.
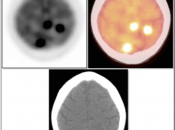
Brain Metastases:
- Far more common than primary lesions (> 10 times).
- If small and at grey-white junction, can be easily overlooked.
- Commonly from lung, breast, melanoma and GI primaries.
CNS Lymphoma:
- Usually very hypermetabolic (FDG uptake is often greater than high-grade gliomas or metastatic lesions).
- Association with immunocompromised status.
False Negatives:
- Low-grade lesions
- Cystic lesions with only minimal soft-tissue component
- Cortical lesions obscured by normal intense brain uptake
- Edema may decrease uptake in a region of tumor
- Lesions < 8.0 mm (beneath the resolution of PET)
False Positives:
- Some benign lesions are FDG-avid (e.g. meningioma, pituitary adenoma)
- Seizure focus (if ictal @ time of FDG injection)
- Some low-grade lesions can be intensely avid (e.g. pilocytic astrocytoma, pleomorphic xanthoastrocytoma)
Crossed Cerebellar Diaschisis:
- May see generalized decreased FDG uptake in the cerebellar hemisphere opposite of a supratentorial abnormality (e.g. tumor, edema, infarct, gliosis).
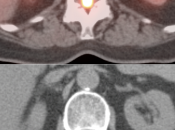
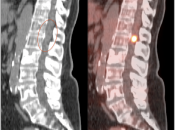
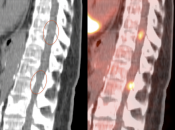
SPINAL CORD:
- Primary lesions are rarely evaluated with PET/CT.
- Metastatic lesions are not uncommon, appearing very focal, with uptake > liver activity.